BOSTON — As an I.C.U. doctor I’m used to giving bad news, but I was not prepared for this.
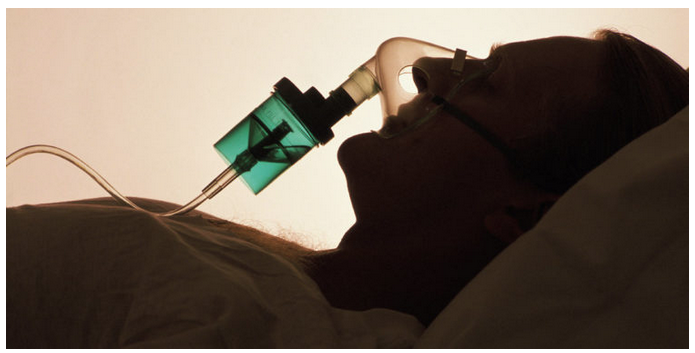
I paused outside my patient’s room to watch her for a moment. She lay on the bed, tethered to a ventilator by the tracheostomy tube in her neck. Her husband sat in a small plastic chair beside her with his hand on her leg, smiling at some silly sitcom playing on the TV. I hesitated a beat. And then I entered.
I had to tell him. There was no way to soften the blow. The hospital is changing its rules, I said. No more visitors. When you leave today, you both need to say goodbye.
I watched their faces shift. My patient’s breathing quickened, and her ventilator alarm sounded. Her husband quickly moved his hand to her shoulder and her breaths slowed; the alarms silenced. He knew how to calm her. He had been there through all of it — hospitalizations for cystic fibrosis, the transplant, the bouts of rejection. When we took away her voice with the tracheostomy tube, he spoke for her.
But now, as we tighten our protocols to protect our patients from the threat of Covid-19, she’s alone. Here in my hospital, as in so many others throughout the country, we’ve banished most visitors. It’s a tough decision that leaves our patients to suffer through their illnesses in a medical version of solitary confinement. And I’m worried for them. Because those of us on the front lines simply don’t have a plan for this.
The isolation is, of course, even more profound for those who are infected with, or are being evaluated for, coronavirus. I took care of one such patient who was intubated when he started coughing up blood on the general medical floor. He was alone in his room, on FaceTime with his daughter, when it started. So that is the last image she has of her father — on a shaky computer screen, blood staining his hospital gown. I offer her updates over the phone, but the truth is that I am not sure when she will be able to see him again.
Or even if she will be able to see him. The devastating image of the lonely deaths of coronavirus patients in Italy hangs over us all. Talking with one of the nurse practitioners in our hospital’s new Covid-19 I.C.U. one recent night, I asked what worried her most. “Patients dying alone,” she replied quickly.
A doctor next to her nodded in sad agreement. On a recent shift, he had intubated an elderly husband and wife, both of whom had severe respiratory failure from coronavirus. Their daughter asked if she could come in to see them. Though we will make exceptions for many end-of-life visits, in this case, he had to say no — they all lived together, the daughter had a fever herself, and as a result could risk infecting other hospitalized patients. Which means that if her parents die of this, they will do so in separate sterile hospital rooms, far from anyone who loves them.
So it’s up to us, the health care workers who are seeing these patients at the front lines, to find ways to maintain connection, to balance our fear with tenderness. This won’t be easy. I think of myself as the kind of doctor who sits at a bedside, who holds a hand, who explains what is going on slowly and gently even to my intubated patients because I can’t know what they will remember. I want to be the doctor who is always willing to spend a few extra minutes despite being stressed or rushed.
But that is not the kind of doctor I have been for the past few weeks. Because I don’t want to spend a moment longer in a Covid-19 patient’s room than I have to. Even with a mask firmly in place, even with a gown and eye protection, I do not want to share the same air. So I do what I need to do and then I leave. I don’t take the time to reassure, to explain, surely not to hold a hand. Truth is, I am scared.
As for keeping families involved from afar, this is not easy either. The number of phone calls we need to make has soared — just as our volume of patients threatens to as well. I can feel how much these conversations matter, in the breathless way a daughter answers the phone when I call, the way a husband asks me to speak slowly, please, so that he can take notes. But time is short. The incessant beeping of our pagers urges us off the phone. We will talk again tomorrow, I say, and I hope it is true.
This is not enough. If this is our new reality, then we must do better. At my hospital, efforts are underway to bring an iPad to the bedside of every patient in isolation for coronavirus. We will also need to practice difficult conversations like delivering end of life news over the phone, without relying on body language and touch and facial expressions to convey meaning.
As critical care doctors, we now understand that our patients and their families carry with them invisible scars from their time in the intensive care unit — anxiety, depression, post-traumatic stress. The words we use matter. And I know that we are overworked and afraid that we won’t have the equipment we need to protect ourselves. But I worry that unless we find some way to mitigate the overwhelming isolation this virus has created, we will leave a fleet of wounded patients and family survivors in its wake.
I was thinking about all of this as I walked through the hospital on my way to the unit the morning after my patient and her husband said goodbye. The family waiting room, often so full that people have to sit on the floor, was empty. I had never seen it like that. A lone coffee cup on the table was the only sign of how things had been just the day before.
I entered the unit, headed to my patient’s room. She was awake already, breathing quickly on the ventilator, eyes wide. When she saw me, she started to mouth words. Her husband would have been able to understand, but her lips moved quickly and I had no idea what she was trying to say. She soon grew frustrated. “I’m sorry,” I told her. But she was done. She closed her eyes and turned away, toward the empty chair next to her bed. I apologized once more and then, as my pager summoned me down the hall, I stepped from the room, leaving her alone.
Daniela J. Lamas is a critical care doctor at Brigham and Women’s Hospital in Boston.
The post When You Die of the Coronavirus, You Die Alone appeared first on New York Times.