
The deadly novel coronavirus is so prevalent in Haiti, where a fever has been raging for weeks, that a top authority on public health is now saying there’s no need to test anymore to declare that someone is infected.
That assessment is stirring debate in medical circles, where some agree that providing symptom-based care is the way to go given the extent of the transmission, and others argue Haiti needs to ramp up testing to contain the spread.
The controversial view also has raised questions about whether Haiti, which has been struggling to manage COVID-19, is becoming so overwhelmed with the rapidly accelerating number of cases that it’s now taking a markedly different approach to the coronavirus than its neighbors and the World Health Organization’s “test every suspected case” directive to contain the spread of transmission.
Since Haiti confirmed its first two infections on March 19, the number of laboratory confirmed cases have spiked to 3,334 with 51 deaths in the population of nearly 11 million. The country, however, has only tested 7,351 suspected cases — far less than the 94,000 performed in the neighboring Dominican Republic, where there are 19,600 confirmed cases and 538 deaths in a population of roughly the same size. Both countries share the island of Hispaniola.
“All patients presenting with symptoms here have over 80 percent probability to have it,” Dr. Jean William “Bill” Pape, co-president of Haiti’s presidential response commission, told the Miami Herald. “Almost all patients with [symptoms] of COVID-19 test positive. Hence no real need to perform the test.”
Pape’s argument is based on his analysis, he said, of cases in the Port-au-Prince metropolitan region. The epicenter of the pandemic in Haiti, the capital region has 80 percent of the confirmed infections. Port-au-Prince is also where Haiti’s only two COVID-19 testing laboratories, GHESKIO, run by Pape, and the other by the government, are located.
A trailblazer in the fight against HIV/AIDS treatment in Haiti, Pape said he’s applying his past experience as a clinician treating acquired immune deficiency syndrome to his approach with COVID-19, which is caused by the SARS-CoV-2 virus and can trigger mild to deadly respiratory tract infections. He was treating HIV positive Haitians at his GHESKIO research and health center for two to three years before a reliable test was available using, he said, just a clinical diagnosis.
Currently, he is treating 31 patients, including six physicians, who have COVID-19. With the exception of two who needed to be hospitalized for low oxygen saturation, all are being treated at home, said Pape, who on Sunday almost lost his downtown GHESKIO site to a raging fire.
“They all are able to monitor their oxygen saturation at home and we are expanding this technology in slums with community health agents. Hence it is necessary to expand a clinical definition of COVID-19,” he said. “It makes it possible to account for them and provide proper care to them. This is the case for all epidemics.”

Pape’s focus on treating patients, rather than trying to find where they are to manage the course of the epidemic, has some fellow physicians and public health specialists wondering if Haiti is throwing in the towel because it cannot meet the growing testing demand as infections surge.
Last month, Pape’s co-president on the commission, Dr. Lauré Adrien, who also is executive director of the Ministry of Public Health and Population, ignited controversy when he told Haitians that there is no “fever epidemic” spreading in the country. There is only COVID-19, Adrien said, and the high body temperatures Haitians are seeing should be automatically linked to the disease.
“They have lost control of the disease,” said Dr. Junot Félix, who runs a health consulting firm in Port-au-Prince and is a critic of the government’s response. “There is no other way to manage an epidemic than to test the people so that you can follow the virus … isolate them and trace and test their contacts.”
He called Pape’s clinical approach, and the declaration by Adrien that all fevers are linked to COVID-19, as “not making any sense.”
“You can’t say someone has a fever and you give them medicine and don’t test them,” Félix said. ”The first thing you need to fight an epidemic is information. … How are you going to manage an epidemic if you do not know where the sick people are and how it’s moving?”
On Friday, the head of the government’s water agency, who had tested positive for the disease, revealed in a radio interview that after months of saying patients needed to test negative to be cleared, the health ministry had changed its protocol, according to his doctor. Patients can now resume normal activities after eight days with no symptoms, Guito Edouard said he was told.
Neither Adrien nor a ministry spokesperson responded to a Herald inquiry seeking confirmation of the change. Two members of the scientific cell advising the government’s response, said they are working on a recommendation to clear patients without a second test — which is still being done elsewhere in the Caribbean — based on studies on when someone is no longer considered contagious. The members acknowledged that Haiti, which has only managed to acquire 19,500 diagnostic tests so far, also does not have enough tests.
Alarming spike in COVID-19 cases
Haiti is still in the early stages of the pandemic, which experts say could peak this summer.
But in just one month, the number of Haitians testing positive for the coronavirus has dramatically increased from 100 cases and 11 deaths on May 4, to 2,924 confirmed cases and 50 deaths a month later, on June 4.
The medical aid group Doctors Without Borders/Medecins Sans Frontieres said while the rise is alarming, the real infection numbers are most likely higher. Official statistics, for example, aren’t capturing those dying undiagnosed for the virus or whose deaths in rural and slum communities, after they’d experiencing COVID-19 symptoms, are going unreported.

In recent weeks, woefully sick and dying Haitians have called the health ministry’s 2020 COVID-19 hotline pleading for help, only to refuse an ambulance from fear of being labeled with the disease by neighbors.
Meanwhile, those seeking treatment at the few available treatment centers are arriving late and in critically ill condition.
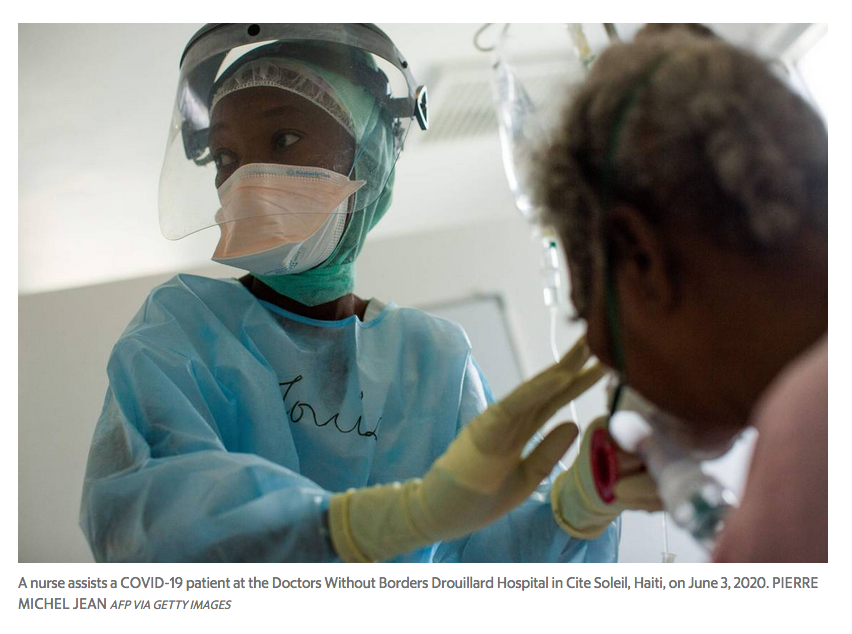
“Unfortunately, a dozen patients have died on arrival at the hospital, and many others have arrived in critically ill condition,” MSF Mission Director Hassan Issa said about its Drouillard Hospital in the Cité Soleil shantytown.
Many with symptoms are not even going to the hospital for treatment, which Issa fears will only fuel the spread in communities and reduce individuals’ chances of survival.
Issa said the problem with Haiti’s official testing data is that it underestimates the extent of the disease in the country where the stigma faced by people increases their reluctance to get tested. He has no issues with Pape’s symptom-based care approach and said at this stage in the pandemic, the strategy “will make it possible to reduce the time taken for treatment and therefore save many more patients.”
The lost public relations messaging
Haiti’s Ministry of Public Health and Population has made no secret about its difficulties in tracing transmission of COVID-19 as uncooperative Haitians resist testing and even refuse to provide names of individuals they may have exposed to the disease from fear of being stigmatized.
And for all intensive purposes, the government has lost the public relations battle in the fight against the virus. While officials have managed to get Haitians to increasingly wear masks in Port-au-Prince, many Haitians are still not doing so outside of the capital and many still do not believe the disease is real, dismissing COVID-19 related symptoms as “a little fever.”
Even the basic message that most people infected with the virus will only suffer mild symptoms and will survive has become lost in the population. Haitians view the virus with shame, credit homemade herbal remedies for saving their lives, or blame anything but the coronavirus for their respiratory symptoms and other telltale signs of infections.
On Sunday, Twitter user Jhoane Boursiquot took to the social media platform to express her frustration over Haitians’ refusal to accept that COVID-19 is real.
“I have a friend from Cap-Haïtien who I wrote to hear news from. He told me, he has a fever, all of his body, his throat ache, he’s lost his sense of taste,” Boursiquot tweeted in Creole. “He added that they seem like symptoms of the coronavirus. I told him it is the coronavirus. He said, ‘No. It’s the fever.’ Oh Lord.”

Whereas most countries in Latin America and all in the Caribbean have enforced some form of mandatory lockdown to slow down transmission, Haiti has done no such thing despite extending a state of public emergency until July. There is no mandatory confinement. The government can’t even enforce its own rules banning large gatherings as mayors around the country complain about nightclubs being overrun with patrons despite an 8 p.m. to 5 a.m. nationwide curfew.
Without proof of infection, even the most well-informed Haitians continue to have a laissez-faire attitude toward the highly contagious disease as people go about their daily lives without any social distancing or confinement measures.
If for no other reason than to convince a population in denial, public health experts say Haiti can’t afford to give up on testing because it’s the only way to persuade Haitians to take the contagion seriously.
‘Herd immunity’
Haiti remains at high risk for a serious outbreak not just because of the population’s attitude toward the disease but the fact that thousands continue to pour into the country every week from the Dominican Republic, despite the closed borders.
With more than 27,000 Haitians returning since the start of the outbreak, according to the International Organization for Migration, Haiti cannot afford to approach COVID-19 blindly, said Carlos Espinal, the director of the Global Health Consortium at the Robert Stempel College of Public Health at Florida International University.
Testing and widespread testing, Espinal said, will allow health officials to know how the virus is moving, the speed of the transmission and what strategies they need to impose, especially in areas where the disease is most prevalent, to reduce the incidence and change the curve.
“You cannot say, ‘Everybody who develops a fever in a country where malaria is so endemic, where you have cholera and many other diseases that produce fever, have COVID-19,’ ” Espinal said. “You will have most of the population infected. It’s not possible to say that.”

The declaration by the health ministry’s Adrien, along with Pape’s clinical approach has led to chatter and concerns among some physicians about whether the country is deciding to go the way of the United Kingdom and Sweden, whose initial approach to the virus was to allow millions of their citizens to get infected in hopes of building a long-term resistance to the disease.
Espinal said such a policy, known as “herd immunity,” would be disastrous for Haiti, which “has a high risk of a serious outbreak” in the coming weeks.
“At the present time we don’t even know if this virus will produce a solid strong immunity after infection,” Espinal said. “There is no proof of the concept to go for herd immunity and wait until you get 70 percent of the population infected to protect the people. There is not a lot of scientific evidence, so they really need to go into the testing of people and people with symptoms. And they need to make an effort to move out of the centralized [testing] area.”
Not enough test kits
Even as Haitians have resisted testing or lacked access, the number of suspected cases sent to the National Laboratory and Pape’s GHESKIO laboratory have been doubling each week.
That also means that the number of available tests is quickly dwindling.
At the current speed of 400 to 500 tests being run a day, Haiti would need access to enough kits to perform about 12,000 COVID-19 tests a month, experts surmise, if it were to decentralize testing and make it available in other cities outside of the capital.
Pape said there are currently 41 machines spread out across the country that could achieve this. But Haiti has nowhere near the required supplies, including reagents, a key chemical to test for COVID-19.
The machines in question were donated by the U.S. Centers for Disease Control and Prevention to allow for one-hour diagnosis of tuberculosis by polymerase chain reaction, the same technique used to detect the coronavirus and then confirm COVID-19. The machines can be used to diagnose COVID-19 in the countryside where today there are few laboratory confirmed cases.

CDC officials did not respond to a Herald inquiry on whether the agency was seeking to assist Haiti, which tried to order 5,000 additional tests from the United States only to have them blocked by President Donald Trump’s signing of the Defense Production Act, a government source said. The order prevents U.S. distributors from diverting personal protective equipment, or PPE, such as face masks and gloves and COVID-19 testing kits, overseas.
The U.S. Agency for International Development, one of Haiti’s biggest donors, said while it has given about $13.2 million in COVID-19 assistance to Haiti, “to date, USAID funds have not been used to procure reagents for COVID-19.”
“But we are continually assessing the needs on the ground and adjusting our response during this pandemic in an effort to support Haiti’s needs,” said Acting USAID spokeswoman Pooja Jhunjhunwala.
As donors decide whether to help, frustrations over the lack of testing and the government’s haphazard approach grow.
Félix, the physician, said many of the decisions being taken by Haiti “aren’t rooted in any logic, or data that they have.”
“Take for example, the curfew they issued. No one can explain to me why there is an 8 p.m. to 5 a.m. curfew. Haitians don’t regularly go out at night. If it’s a problem with clubs, close the clubs,” he said. “Once 5 a.m. arrives, everyone takes to the streets and does what they want. Does this virus only function at night?”
Earlier this month, the Pan American Health Organization, the WHO’s regional office for the Americas, warned of a “pending humanitarian crisis” in Haiti. On Friday, PAHO said these concerns remain valid and re-emphasized PAHO Director Dr. Carissa Etienne’s call for all countries in the Americas region to ramp up testing so as to not lose control of the transmission.
“The health system in Haiti has limited capacity to deal with an outbreak of COVID-19,” PAHO spokeswoman Ashley Baldwin told the Herald in a statement. “There are few beds for treating COVID-19, insufficient number of health care professionals and insufficient personal protective equipment. The security of the COVID-19 designated hospitals and the safety of community health workers is also of grave concern.”

Espinal, the FIU global health expert, said the situation in Haiti should be of concern for everyone. If Haiti can’t afford to access more tests, then PAHO needs to help, said Espinal, adding that the situation in the French-speaking Caribbean nation is akin to that of Nicaragua.
PAHO has publicly chided leaders in the Central American nation for their lack of social distancing measures, and low test numbers.
“No one knows exactly what’s going on, but people are dying without diagnosis and no access to healthcare and there is very little that we know,” Espinal said of Haiti. “If they don’t have surveillance, if they don’t have data, and if they don’t have any strategy on social distancing or mandatory confinement of the key areas where they are finding most of the cases, within weeks we will have a critical, chaotic situation in Haiti.”
