 As Liberia, Sierra Leone and Guinea look at ways to repair holes and strengthen their health systems in the wake of Ebola, we spoke with Equal Health’s Nadia Raymond – a Haitian-born nurse who shared her thoughts on access to health after Haiti’s earthquake and cholera outbreak
As Liberia, Sierra Leone and Guinea look at ways to repair holes and strengthen their health systems in the wake of Ebola, we spoke with Equal Health’s Nadia Raymond – a Haitian-born nurse who shared her thoughts on access to health after Haiti’s earthquake and cholera outbreak
Ebola Deeply: Nadia, you were born in Haiti and grew up in the U.S. What were your observations when you first went to work as a nurse in Haiti?
Nadia Raymond: When the 2010 earthquake happened in Haiti, one of the first things I did to help was to go to Haiti and work side by side with the Haitian nurses to understand the challenges. Because I came to the U.S. at the age of 17, I didn’t fully understand the nuances of the Haitian health system. But this experience enabled me to collaborate with my Haitian colleagues and really learn the culture of the health care system. I can say that’s one of the best decisions I made because it allowed me to both see and experience, as well as understand, what the patients needed and how best to assist the medical professionals to provide care.
“To make sustainable changes we need to take into account traditions, beliefs and hierarchy”
Seventeen days later, when I returned back to the U.S., I remember feeling that I did not do enough. I wanted to make a greater impact. Sometimes volunteers go to a foreign country to offer help and may judge the local professionals that are providing care. It is only when you’ve walked in their shoes that you see how dedicated they are and understand how defeated they can feel.
Ebola Deeply: What are the biggest challenges for health workers in Haiti currently?
Nadia Raymond: The care they would like to provide is compromised because of the lack of supplies as well as lack of staff. They’re fighting an uphill battle on a daily basis. In the last five years, I’ve worked closely with nurses in Haiti to see how together we can change the shape of health care delivery as well as encourage nurses to find their voices. To make sustainable changes we need to take into account traditions, beliefs and hierarchy within the culture and find new approaches that will complement and improve the work.
“Community health workers are a great gift to health systems”
It’s about teamwork, rather than a situation where things are broken up into silos – where everybody is doing their own thing. The new generations of medical practitioners in Haiti are starting to acknowledge the need to be at the table together: doctors, nurses, physical therapists, social services, whatever might be needed at that particular time. It’s often difficult to see the progress when the problem is so massive, so you actually have to be on the ground working and experiencing to see the changes.
Ebola Deeply: One of the most successful mechanisms for curbing the Ebola outbreak was the impact of community health workers. Is that also the case in Haiti?
Nadia Raymond: There has been a culture shift in the last couple of years about how we educate community health workers in Haiti. I remember when the cholera outbreak happened, it was the community health workers that really went around to the villages and educated people on interventions like handwashing. That made all the difference in slowing down the outbreak. Community health workers are a great gift to health systems – especially if they are trained properly on prevention.
Ebola Deeply: Haiti still has a long way to go, but what have you learned about health system strengthening that could also be applied to other contexts?
Nadia Raymond: The important lesson learned is that no one organization or person can do it alone. A health care system is a chain. If you take one link out, it will fall apart. In countries with advanced health care systems, there is almost always some kind of collaboration going on.
One of the major lessons that I’ve learned – although I think this is changing – is that some organizations go to countries and essentially say, “I’m here to rescue you.” And then they go there, do it and leave the population with nothing. You do not reach the root of the problem, and to do that you need to understand the culture, the way they operate, the way they function, how they treat each other, how they relate and communicate. It’s different in every culture.
How do you have better outcomes? If only one person is making the decisions and not taking everyone else into account, you’re not going to have very good outcomes. You may have adequate outcomes for a while, but once you step out, it will fall apart. Among the many things that are working now in Haiti, HUM (Hopital Universitaire de Mirebalais) which is the result of a partnership between the Ministry of Health in Haiti and Partners In Health. Equal Health, the non-profit organization I work with, is another great example of a team of health care professionals working together to improve health care delivery in Haiti.
Better and sustained outcomes will become a reality when we ask these questions, “How can we modify it to your culture, your reality?” “What do we need to do to fix our plan to help you grow?” It’s not just a matter of taking it and putting it in place. “How do we make it work for you?” For us to be able to be successful at that, we have to reach out to our partners and come together at the table and discover what works. One of the many lessons that I’ve learned is the importance of continuous collaboration and active listening.
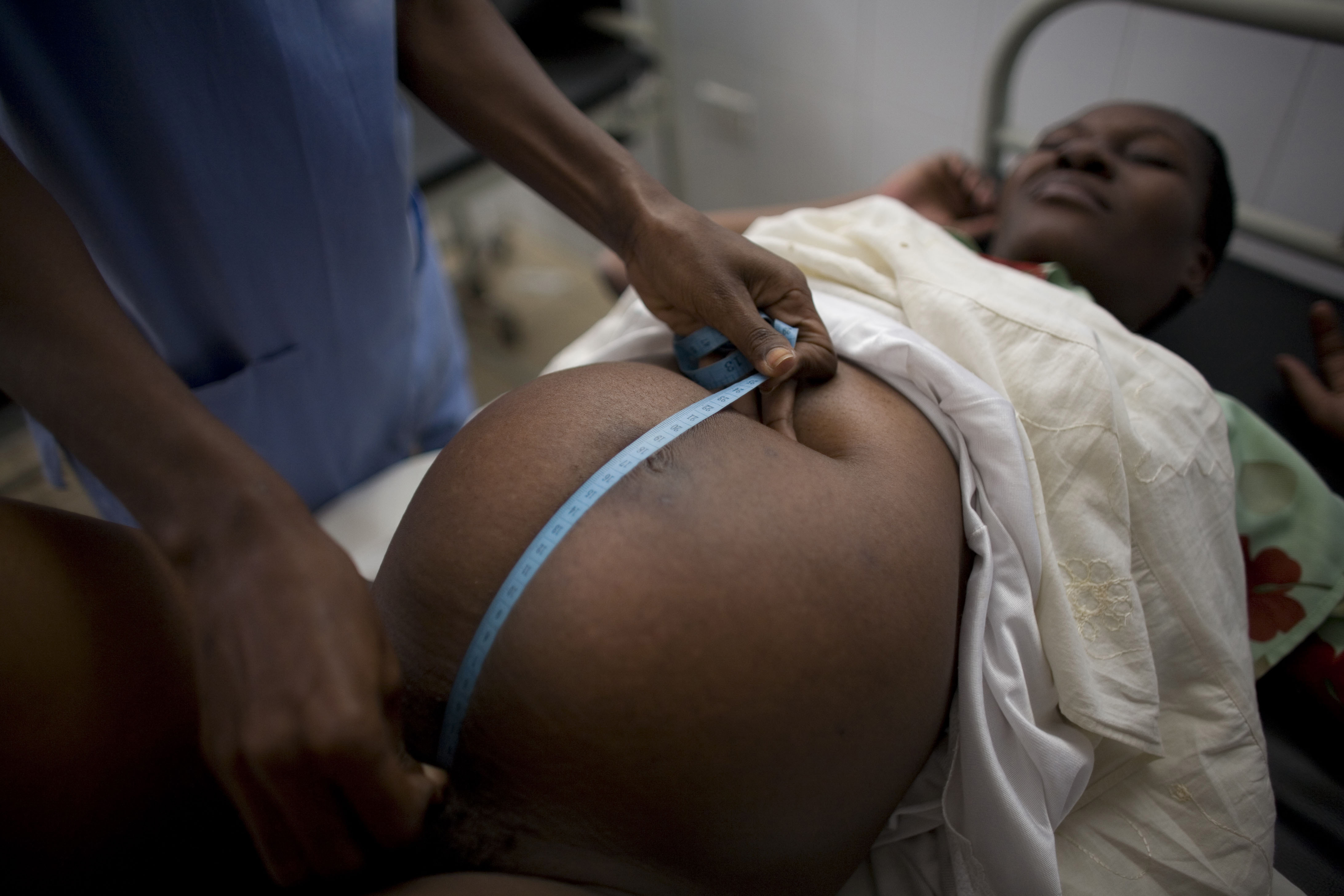
File photo by Associated Press/Ariana Cubillos